With the untimely death of the Ironman, Dean Mercer, at the age of 47, we are strongly reminded of the frailties of our existence and the clear point that no one has a 100% guarantee of a long life, despite following healthy lifestyle principles. Dean, allegedly, died of a cardiac arrest whilst driving and I am not privy to his autopsy results (at the time of writing this report). The media, incorrectly, reported Dean died from a heart attack. Although this may have been the cause, there are many other causes of sudden cardiac death, both in elite athletes and the less fit members of the general public.
Although it is not rare for a younger person to suffer a heart attack (which is where a fatty plaque in the wall of an artery suddenly ruptures, blocking the artery), there is also the possibility of a number of other cardiac and at times, non-cardiac conditions, causing a cardiac arrest, which is where the heart actually stops pumping.
The commonest cause of death in people below the age of 40 is, in fact, hypertrophic cardiomyopathy, a genetic, excessive thickening of the heart muscle which often, under conditions of stress, such as excessive exercise, emotional stress or the use of legal or illegal drugs, may irritate the heart to the point of cardiac arrest.
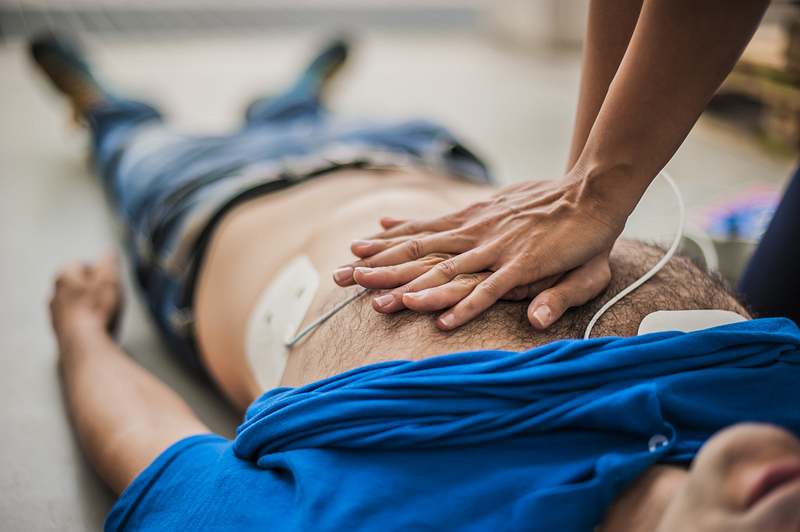
So, the big question here is how do we determine who is at risk for any of the number of conditions that may lead to a cardiac arrest? The answer here is that in certain cases it is not possible. We have screening tests for the most common conditions but even then, they are never 100% accurate and are not designed to detect many of the less common causes.
I am a strong advocate of coronary calcium scoring which is a non-invasive, no dye, no injection, snap shot of the coronary arteries in the heart, using a CT scan that as the name suggests, measures in a quantitative fashion, the amount of coronary calcium in your arteries. This is an indirect marker for the amount of fat and basically assesses cardiac risk. The higher the coronary calcium, the higher your risk. But, regardless of cardiac risk, the younger you are, the less calcium you have.
0-low risk
1–10-trivial
10–100-mild atherosclerotic load
100–400 — moderate risk
> than 400-high risk
But, any calcium in a person below age fifty is too much. So, a coronary calcium score of 20 in a 45-year-old is much more serious than a score of 200 in a 70-year-old. Also, coronary calcium is almost always only an indicator of common, garden variety coronary atherosclerosis and does not detect hypertrophic cardiomyopathy, inflammation, clotting potential and many other early cardiac issues.
The entire issue of what causes and how to prevent sudden cardiac death is far too complex to cover in a single article but tragic incidences, such as the death of a prominent Australian Sports Star, does require a healthy debate but often raises more questions than answers.
Although we all know exercise is very beneficial, is there a point where more is not better? Increasing evidence seems to be pointing to the fact that 3–5 hours per week of moderate exercise is the right dose and beyond that does not help but, of course, the greatest risk is being inactive. What factors actually precipitate an event? Often people suffer the cardiac arrest after vigorous exercise, not during. Many people die during sleep, raising the spectre of sleep apnoea and other sleep associated disorders. What part does any stressors (combined with vigorous exercise) contribute to a cardiac arrest? Here I am referring to other forms of physical stress such as an intercurrent illness (do not perform heavy exercise when you have a virus); emotional and mental stress; pharmacologic stress — legal and illegal — e.g. exercising following strong coffee; a night out on the grog; having recently used illegal drugs et cetera et cetera.
Although this is definitely not a comprehensive analysis of sudden cardiac death, this clearly shows that a visit to your general practitioner to have your blood pressure checked, a few simple blood tests such as cholesterol, blood sugar levels and possibly a basic ECG is a very inadequate screen for serious cardiac conditions.
As a preventative cardiologist, I treat each case on its own merits, investigate and treat accordingly. I believe it is possible to screen for, manage and potentially prevent most common illnesses but unfortunately there will always be the occasional patient who, despite all best intentions will still “fall through the cracks”, so to speak. It is not the doctor or the patient’s fault, it is the disease’s fault combined with the environmental and genetic circumstances underlying that particular person and disease.
